#ศาสตร์เกษตรดินปุ๋ย : ขอบคุณแหล่งข้อมูล : หนังสือพิมพ์ The Nation.
The day Juliet Daly’s heart gave out started much like every other Monday during the quarantine.
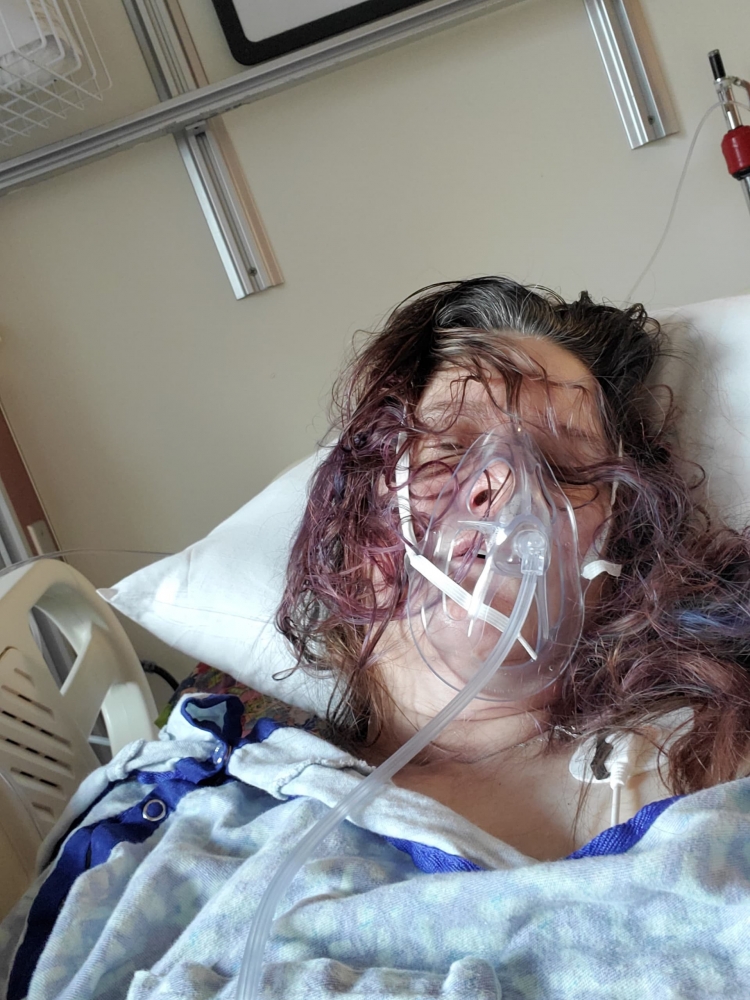
The 12-year-old from Covington, Louisiana, padded out of her room in her PJs shortly after 7 a.m., ate a half-bowl of Rice Krispies, and got on a Zoom call with her sixth-grade social studies class. She had been feeling unwell all weekend with twisting abdominal pains, vomiting and a fever of 101.5, but she seemed to be on the mend.
The weird thing, she recalled, was that her lips looked bluish in the mirror and she was super tired. In fact, she kept falling asleep unexpectedly. On the couch. In front of her computer. In the bath.
“I thought I was feeling a bit better,” she said, “but I couldn’t keep my eyes open.”
With all the news swirling around them about the pandemic, her parents, Sean and Jennifer Daly, had been monitoring their daughter’s illness closely. She had been healthy and did not have a cough, shortness of breath or other typical symptoms of covid-19, so Jennifer, a radiologist, initially suspected appendicitis, some kind of stomach bug, or perhaps the flu.
That afternoon, they took Juliet to the emergency department, where doctors noticed an unusual constellation of symptoms pointing to a different problem. Her heart rate was extraordinarily low, jumping around in the 40s when it should have been between 70 to 120 beats per minute. And when they squeezed her nails, they turned white and stayed white when they should have gone back to pink.
Juliet was in a kind of toxic shock, and her heart had become so inflamed it was barely beating.
It was still relatively early in the outbreak, April 6, and the hospital hadn’t seen other children in this condition. But the doctors knew enough about the pathogen’s effects on adults that they immediately suspected the coronavirus.
– – –
Cases like Juliet’s, a puzzling inflammatory syndrome in children believed linked to covid-19, had been popping up in different parts of the world for months, but it wasn’t until recently that health authorities began tracking the phenomenon.
The number of infected children, while still small, is estimated to be a few hundred – larger than anyone anticipated for a disease thought to inflict little, if any, harm on children. Doctors in Britain and Italy had issued alerts in April, and the American Heart Association warned last week that some pediatric patients “are becoming very ill extremely quickly,” urging providers to evaluate them right away.
On Thursday night, the Centers for Disease Control and Prevention issued an advisory and gave the unusual condition a name – multisystem inflammatory syndrome in children, or MIS-C.
More than 100 children are believed to have it in New York state, with about half in New York City, where three have died. In recent days, medical centers in 14 other states have reported similar cases. Scientists still believe most children and young people experience only mild illness or none at all if they become infected with the coronavirus. But they’re concerned about the critical nature of the inflammatory syndrome cases, which seem to be appearing in children weeks after a wave of infections in their communities.
“We’ve been seeing kids steadily for two months,” said Roberta DeBiasi, infectious disease specialist at Children’s National Hospital in the District. “But this presentation is clearly different. It’s not that we just didn’t notice this before. It’s a new presentation. And the fact that it’s happening two months after the initial circulation of the virus gives weight to the idea that it’s an immune-mediated phenomena.”
Jennifer Owensby, a pediatric intensivist at Rutgers’s Robert Wood Johnson University Hospital in New Brunswick, New Jersey, said the first group of children she saw with covid-19 appeared to have classic respiratory symptoms, such as shortness of breath. Now, she said, “The vast majority are coming in with symptoms of cardiac failure, which is extremely rare in pediatrics, especially in normal, healthy kids – which is why this is so alarming.”
Writing in the Lancet medical journal this week, Italian doctors reported on a cluster of 10 children struck with the inflammatory condition in the coronavirus epicenter of Bergamo. The cases appear to have characteristics of an illness first identified in Japan known as Kawasaki disease, which causes inflammation in blood vessels and includes a persistent fever. But these children were older than is typical with Kawasaki, which usually strikes those younger than 5, and they had more serious heart issues.
Just like Juliet, who is among the first known children in the United States to develop multisystem inflammatory syndrome.
– – –
Sean Daly was at the hospital with “Jules,” as he sometimes called her, while Jennifer was on the phone from work.
A transportation planning consultant with no medical background, Sean remembers feeling confused as doctors told him they were giving his daughter an epinephrine drip to help her heart, and were sending her to a larger hospital with more expertise and equipment. They said they would put her on a ventilator to stabilize her for the helicopter trip to Ochsner Medical Center, about 50 miles away in New Orleans.
Sean, unaware of the gravity of his daughter’s condition, thought ridiculous thoughts about the absurdity of his shorts and flip-flops amid the alien-looking hospital workers in head-to-toe protective equipment. And he thought about how, just a few minutes earlier, his daughter had been well enough to walk across the parking lot and into the ER. He heard an announcement about something called a “code blue” and wondered why more and more people kept rushing into her room.
When the attending doctor finally popped out, Sean recalled, she was shaking. She said Juliet had gone into cardiac arrest, and it took them nearly two minutes of CPR, or cardiopulmonary resuscitation, to revive her.
“It didn’t process all that well with me,” he said. “She was telling me Juliet was ‘back,’ and I was like, ‘That’s good. I didn’t know she had gone anywhere.’ Thankfully I was not in the room. I don’t think I would have handled that.”
Jennifer was hysterical.
“It was horrific. It was beyond anything. It was shocking how quickly it happened,” she recalled.
– – –
When Jennifer arrived at Ochsner, she didn’t understand how she could have possibly beaten her daughter there. She had driven for about an hour in a semicircle around Lake Pontchartrain while Juliet had been airlifted.
“I was crying and freaking out,” she recalled. By the time she was able to grab a nurse, she feared the worst. “I just need to know one thing now,” she demanded. “Is she alive?”
Juliet’s helicopter had been delayed because she had coded a second time and, again, doctors restarted her heart. But by the time they wheeled her into the pediatric intensive care unit in the new hospital, some of her other organs had begun failing, too, probably because the heart was unable to pump the oxygen-filled blood they needed.
Juliet’s liver and kidneys were in shock. There was blood in her lungs. Her pancreas was inflamed.
Heartbeats are controlled by electrical impulses that travel down the right and left branches of the heart at the same speed. Somewhere in Juliet’s heart, a block was causing the system to go haywire.
A team of pediatric cardiology specialists gave Jennifer a name for her daughter’s condition: acute fulminant myocarditis – a sudden onset of heart failure, shock or life-threatening arrhythmias.
The doctors began medications, requisitioned a heart bypass machine in case it was needed, and prepared Jennifer for the possibility that Juliet might need a transplant.
“They were not sure she was going to make it the first night,” Jennifer said. “It was a total nightmare.”
Meanwhile, Juliet’s nasal swabs came back positive for the coronavirus and adenovirus, one cause of the common cold. The results were bewildering because none of the other family members – Sean, Jennifer or Juliet’s brothers, ages 5 and 16 – had been the least bit sick. But if her condition was post-viral, occurring weeks after infection – as scientists increasingly suspect in such cases – there were any number of ways she could have been exposed, since school had still been in session and stay-at-home orders had not yet been issued.
Since none of Juliet’s family had symptoms and test kits were in short supply in the area, doctors opted not to test them.
After confirming the coronavirus diagnosis, doctors gave Juliet an immunoglobulin product used successfully on Kawasaki patients. They ruled out using hydroxychloroquine, the anti-malarial touted by President Donald Trump, because they were worried about cardiac side effects given her already fragile heart condition.
As Jennifer sat in the room with full protective equipment, including a face shield, mask and gown, she held her daughter’s hand. Only one parent was allowed, so Sean stayed at home with the boys.
Unable to sleep, Jennifer started a group text chat so she could keep family and friends updated. She played Juliet’s favorite song – Maroon 5′s “Moves Like Jagger” – vowed to be as optimistic as possible and prayed.
– – –
That first night was torture. Juliet’s heart was starting and stopping, beating too fast and then too slow, as doctors adjusted the medications. But within 24 hours, almost miraculously, she seemed to be stabilizing. The numbers on her labs for her kidneys and liver were moving in the right direction, and the echocardiogram of her heart had improved.
While Jennifer joked with her husband about Juliet being a heavy sleeper, there were instances when her daughter woke up and seemed to understand her completely.
“We love you,” Jennifer would say. “You’re going to get better.”
She talked about an Easter egg hunt she would have in the yard with her brother, Dominic.
Juliet was able to give a thumbs up and squeeze her hand.
“I’m optimistic she is neurologically intact,” Jennifer texted to Sean. Her tone was clinical, but it had been one of her worst fears as a mother.
By Thursday, doctors were confident enough in Juliet’s progress that they took her off the ventilator, letting Juliet breathe on her own. She was still on a lot of medications and confused and upset about all the tubes coming out of her body.
Jennifer remembers reassuring her she was safe in the hospital, but that she was still very sick and weak.
Juliet’s reaction wasn’t what she expected: “No Mommy, I’m not weak. I’m strong!”
“The first day of regaining consciousness, I was freaking out. I wanted to go home badly,” Juliet recalled. She said she was terrified of how everyone kept stepping on all her cords, which were tangled and plugged in outside because the nurses wanted to limit how many times they came into her room. The Band-Aid on her neck was “way too sticky for humankind.” And she could taste the saline they were giving her via IV, and it was bad.
Then on April 15, almost as suddenly as she had been admitted nine days before, doctors told Juliet she was well enough to go home.
– – –
Juliet has no memories of when her heart stopped twice, and her parents are grateful for that.
She was discharged on four medications – two for the heart, a blood thinner and one for her pancreas – but bounced back physically in no time. She was able to return to her school’s online classes, in which she’s continuing her streak of As, and has no trouble riding her bike around the neighborhood.
Doctors monitoring her closely say the drugs are temporary and that they are hopeful she’ll make a full recovery. On Friday, she returned to Ochsner for the first time since her hospitalization for a one-month follow-up appointment. Jake Kleinmahon, the pediatric cardiologist who is treating her, said he was thrilled when the echocardiogram of her heart looked “completely normal.” Like other children with myocarditis, she is restricted from competitive sports for six months (Juliet’s parents say that’s not a problem as she doesn’t really like to sweat) but is otherwise free to engage in activities.
“I do not expect her to have any long-term complications or limitations, even though she came in so severely ill,” Kleinmahon said. “She is quite a fighter and such a brave young girl.”
The only odd change, Juliet said, is that she came out of the hospital with a monster craving for bacon, which she didn’t love before. And she no longer wanted doughnuts, which had been among her favorite foods. Such changes in taste are not uncommon after ICU stays, doctors say.
The emotional part of her recovery has been more challenging. Juliet thinks about other kids who might become sick with the same syndrome. She says she would advise them “not to freak out too much because freaking out makes things worse. Because that’s what I did, and that didn’t help at all.”
She worries more about her family and friends, their future and hers, and the strange world of viruses she knew nothing about before.
“I feel like I’m a bit self-conscious about my body because I don’t know what’s going to happen next,” she said. “I’m worried about how there’s a lot of other stuff you can get.”