#SootinClaimon.Com : ขอบคุณแหล่งข้อมูล : หนังสือพิมพ์ The Nation.
Pandemic is pushing America’s 911 system to breaking point, ambulance operators say
Health & BeautyDec 04. 2020 EMS and firefighters in Washington D.C. prepare for a shift. MUST CREDIT: Washington Post photo by Jahi Chikwendiu
EMS and firefighters in Washington D.C. prepare for a shift. MUST CREDIT: Washington Post photo by Jahi Chikwendiu
By The Washington Post · William Wan
The coronavirus pandemic has pushed America’s 911 system and emergency responders to a “breaking point,” with ambulance workers and their services financially strained.
Ambulance providers from New York to Iowa to Georgia say the situation is increasingly dire. Desperate for a financial infusion to keep such operations afloat, the American Ambulance Association recently begged the Department of Health and Human Services for $2.6 billion in emergency funding.
“The 911 emergency medical system throughout the United States is at a breaking point,” Aarron Reinert, the association’s president, wrote to federal health officials in a Nov. 25 letter obtained by The Washington Post. “Without additional relief, it seems likely to break, even as we enter the third surge.”
The strain could result in longer wait times and some providers going out of business, ambulance operators said.
Ambulance providers are struggling to meet surging demand even while grappling with increased costs of personal protective equipment, overtime, staff shortages as workers fall ill and decreases in the type of emergency calls that are reimbursed.
“There are services going out of business and many right there on the brink,” said Steven Vincent, vice president for Gold Cross EMS, which serves a region of roughly 400,000 people in Augusta, Ga.
While billions have flowed to hospitals and other parts of the health-care system, the nation’s ambulance and emergency responders have received only a tiny fraction of that funding.
Nursing homes and assisted-living facilities received $7.4 billion from a relief fund passed by Congress earlier this year. Rural hospitals and clinics received $11 billion. By comparison, ambulance providers and suppliers received only $350 million, according to the association’s letter.
In interviews, ambulance operators say their workers are exhausted and their managers increasingly struggling to keep operations afloat in the face of a series of financial blows.
Even before the pandemic, the nation’s 911 system was strained. Across the country, 911 calls are answered by a patchwork of nonprofit, for-profit, hospital-affiliated, fire department and municipal-run services.
To make ends meet, some companies – especially smaller ones – relied on fundraisers like pancake breakfasts run by volunteers that are no longer possible amid the pandemic, said Linda Frederiksen, executive director for MEDIC EMS, a nonprofit provider in Davenport, Iowa.
“The system was strained to begin with. Now you’re stretching it even further and the worry is when things start to give,” she said.
As some ambulance services go out of business, others from neighboring counties will have to cover those areas, industry leaders said. To cut costs, some may keep fewer ambulances in the field. Both scenarios would result in longer wait times. Rural areas, which already struggle with wait times and coverage, could be especially hard hit.
“And for some providers, the strain means delaying replacing aging ambulances and equipment,” said Tristan North, senior vice president of government affairs for the American Ambulance Association. “We’re harming our EMS system, not just during covid but for the future.”
Under the quirks of the U.S. health care system, while ambulances respond to all manner of 911 calls, they are often only reimbursed when they transport people to the hospital.
During the pandemic, calls for medical help in many areas have surged, by several hundredfold, in some cases, but those resulting in transport to hospitals have fallen.
As hospitals throughout the country become overwhelmed, many ambulance services have been told to treat patients in place whenever possible and transport only the most acute cases to protect hospital capacity.
In New Rochelle, N.Y., for instance – one of the country’s earliest epicenters for virus – 911 calls for medical help that didn’t result in transport increased from 500 to 6,049 this year. Meanwhile, transport volume declined 25%.
At the same time, operation costs have ballooned. Providers are having to disinfect ambulances after each call and provide testing for their staff. PPE has been expensive and hard to find.
Vincent said the company supplying gloves to his ambulance service in Augusta, Ga., recently informed him it was going to double the price for each case of gloves he orders.
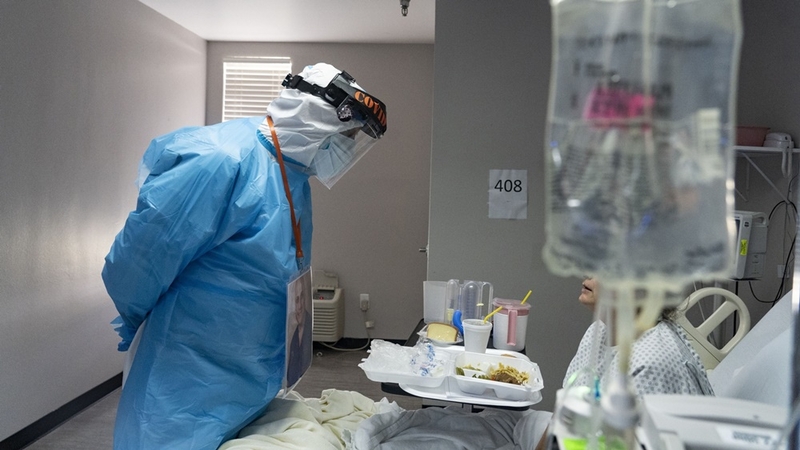
EMTs are often the first health care workers to interact with infectious coronavirus patients. They are the ones who put a mask on patients before they even enter hospitals. And many ambulance workers have been hard hit by the virus.
Vincent said his ambulance service has roughly 85 people working each day. But it has an average of eight to 10 staffers out each week – either because they are sick, or are forced to quarantine because someone in their family is infected.
“There’s been a lot of attention and resources paid to hospitals and nursing homes,” he said. “But for the ambulance workers, there’s a sense we’ve been forgotten.”

 Angela Hunter
Angela Hunter  Dr Yong Poovorawan
Dr Yong Poovorawan  Maryland Gov. Larry Hogan holds a news conference Tuesday on the coronavirus pandemic. State officials on Wednesday discuss plans for distributing a vaccine, saying they will prioritize health-care workers. MUST CREDIT: Washington Post photo by Jonathan Newton
Maryland Gov. Larry Hogan holds a news conference Tuesday on the coronavirus pandemic. State officials on Wednesday discuss plans for distributing a vaccine, saying they will prioritize health-care workers. MUST CREDIT: Washington Post photo by Jonathan Newton 
 On the road outside rural Wessington Springs, S.D., where 1 in 37 people had the virus this month. MUST CREDIT: Photo for The Washington Post by Jenn Ackerman
On the road outside rural Wessington Springs, S.D., where 1 in 37 people had the virus this month. MUST CREDIT: Photo for The Washington Post by Jenn Ackerman